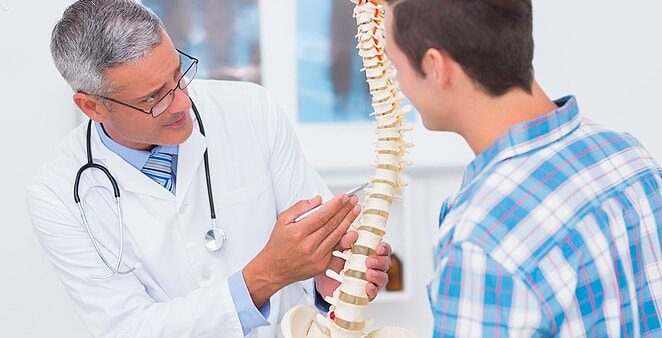
Spinal stenosis is a scary name for what can become a frightening condition. In layman’s terms, it is when your spine narrows to the point of putting pressure on your spinal cord. According to the American College of Rheumatology, spinal stenosis is typically a result of osteoarthritis, which is why the vast majority of cases occur in patients over the age of fifty. The Mayo Clinic explains that osteoarthritis results from wear-and-tear damage, which can lead to the formation of bone overgrowth along the spine. It is this overgrowth that causes the narrowing of the space given to the spinal cord and the eventual “pinching,” which produces the symptoms associated with spinal stenosis. To learn what your options are for spinal stenosis surgery, reach out to Dr. Yashar today.
Symptoms of Spinal Stenosis
The symptoms of spinal stenosis can be difficult for an everyday person to recognize, as it primarily affects the nervous system away from the site of the damage. Although Johns Hopkins Medicine does note that back pain can be a symptom, most patients present with one or more of the following:
- Numbness in the extremities: It could present as a loss of feeling or simply a tingling in the hand, arm, foot, or leg.
- Weakness: Having trouble performing tasks that would normally be easy for you.
- Cramping: Particularly in the legs. This often also results in a pain that radiates down the leg.
- Loss of bowel, bladder, and/or sexual function.
All of these symptoms point to a communicative failure in your nervous system, which could originate from spinal stenosis. However, your doctor will need additional tests to be sure.
Spinal Stenosis Testing
An x-ray to check for bone overgrowth in your spine will be the first stop. From there, your physician may request a variety of scans, including a CT (computed tomography) scan, an MRI (magnetic resonance imaging), and/or EMG (electromyogram) to check the effect on your spine and extremities. If it is determined that you do have spinal stenosis, there are a variety of treatment options available to you.
Spinal Stenosis Surgery
As with any spinal condition, treatment can be a tricky business as the options vary widely from medication to surgery.
With minor cases, medication is the most common option. Physicians can use anti-inflammatories as well as pain medications to keep you comfortable, but they will likely also encourage regular exercise in order to keep your arms and legs strong enough to improve your quality of life.
In more severe cases, which can threaten a patient with permanent paralysis, spinal stenosis surgery may be your only option. Dr. Yashar is an exceptional neurosurgeon in Beverly Hills with a specialization in spinal surgery. For patients exhibiting more advanced spinal stenosis, there are generally three approaches a specialist can take: laminectomy, fusion, or laminoplasty. These procedures vary slightly depending on whether the compression is affecting the lumbar (lower back) or cervical (upper back) portion of the spine, but each procedure works toward a similar goal using a specialized method.
Surgeries
Cervical laminectomy or Lumbar laminectomy: Both of these procedures aim to decompress the area putting pressure on the spinal cord. In these cases, a small portion of the bone (lamina) is removed in order to give the cord room to decompress and heal.
Anterior Cervical Discectomy and Fusion (ACDF) or Lumbar Interbody Fusion: These procedures actually remove the problematic bone and replace it with a spacer. The spacer promotes healing and effectively fuses the vertebra together with the help of screws, plates, and rods in an effort to further stabilize the spine.
Cervical Laminoplasty: Unlike a laminectomy, this procedure does not remove this portion of the bone. Instead, Spine.org explains that, in this case, the operating surgeon makes small cuts on both sides of the lamina, allowing to act something like a hinge. The surgeon moves the bone into a more “open” position, allowing the spinal cord to decompress. A spacer is then inserted to keep the channel open for the spinal cord.
All of these procedures have inherent risks, so it is vital that you speak to a surgeon with an impeccable record who shows you the empathy you deserve. Discuss your options, and do what is best for your own well-being.